SSEP, VEP & BAER Evoked Potential Tests in Queens & Long Island
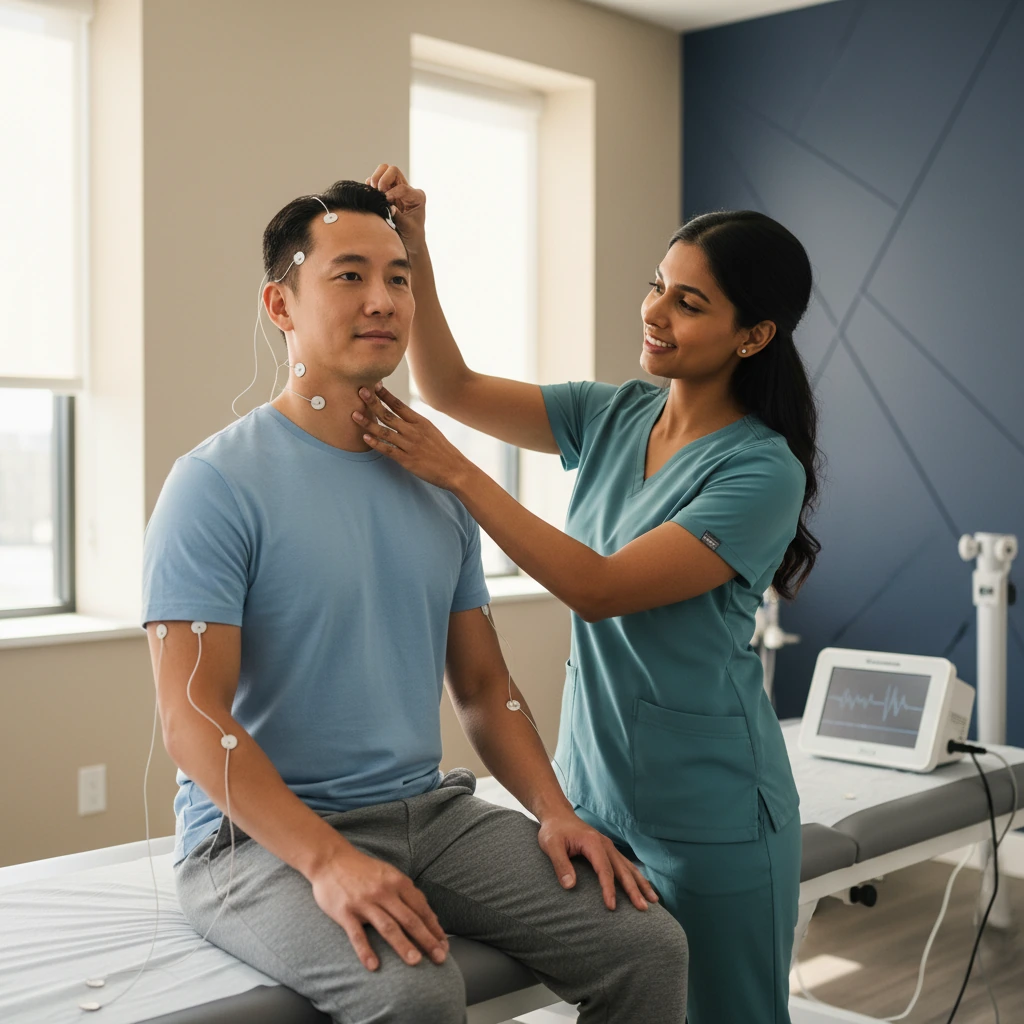
Measuring How the Brain Receives Signals from the Body, Eyes, and Ears - Non-Invasively
Evoked potential (EP) tests measure the electrical activity generated in the brain and along the nervous system in response to specific sensory stimuli. Unlike EMG and nerve conduction studies - which assess the peripheral nervous system from the nerve root outward - evoked potentials test the entire sensory pathway from the peripheral nerve, through the spinal cord and brainstem, all the way to the cerebral cortex. They are the only electrodiagnostic tests that can directly assess the integrity of the central nervous system pathways.
Three distinct evoked potential tests are offered at Dynamic Physical Therapy: Somatosensory Evoked Potentials (SSEP), which test the body's touch and vibration pathways; Visual Evoked Potentials (VEP), which test the optic nerve and visual pathway; and Brainstem Auditory Evoked Responses (BAER), which test the auditory nerve and brainstem pathways. All three tests are completely non-invasive - using only surface scalp electrodes and a specific sensory stimulus - and take 30 - 60 minutes each. They are performed in-clinic, with results integrated into your diagnostic and treatment plan on the same visit.
The Key Distinction: Central vs. Peripheral Nervous System Testing
EMG and nerve conduction studies (NCS) test the peripheral nervous system - the nerves from the spinal cord outward to the muscles and skin. Evoked potentials test the full sensory pathway including the central nervous system - from the peripheral nerve, through the posterior columns of the spinal cord, through the brainstem, and up to the somatosensory cortex of the brain. This means evoked potentials can detect lesions in the spinal cord, brainstem, and brain that NCS and EMG cannot reach. They are the electrodiagnostic tests of choice when spinal cord injury, multiple sclerosis, central demyelination, or brainstem pathology is suspected - complementing both peripheral nerve testing and structural MRI imaging.
SSEP, VEP, and BAER - Three Pathways, Three Answers
Each evoked potential test targets a different sensory pathway and answers a different clinical question. Understanding which test is appropriate requires identifying which sensory system's integrity needs to be objectively confirmed.
Somatosensory Evoked Potentials
Tests the pathway from peripheral nerves in the limbs, through the spinal cord's posterior columns and brainstem, to the somatosensory cortex - the brain region that processes body sensation.
Visual Evoked Potentials
Tests the pathway from the retina, along the optic nerve and optic radiation, to the primary visual cortex - assessing the functional integrity of the entire visual sensory pathway.
Brainstem Auditory Evoked Responses
Tests the pathway from the cochlea (inner ear) through the auditory nerve (8th cranial nerve) and brainstem auditory pathways - the acoustic brainstem pathway from ear to midbrain.
The Four Properties That Make Evoked Potentials Irreplaceable in Diagnosis
Evoked potential tests occupy a diagnostic niche that no other test - not MRI, not NCS, not clinical examination - can fill on its own. Four properties make them uniquely valuable in the diagnostic evaluation of neurological conditions.
In clinical practice, evoked potentials are most powerful when used alongside MRI and peripheral nerve testing - each tool revealing a different dimension of the same pathological process. The combination of a structurally normal MRI with an abnormal SSEP, for example, definitively establishes a functional conduction problem that the imaging alone would miss.
Detects Subclinical Lesions
Evoked potentials can detect lesions in the CNS sensory pathways before they produce any clinical symptoms - particularly in MS, where delayed SSEP or VEP latencies may be the first objective evidence of demyelination. This detection of silent lesions is essential for MS diagnosis, which requires evidence of disease dissemination in space and time.
Measures Function, Not Just Structure
MRI reveals anatomy - it can show a demyelinating plaque, a tumour, or a disc herniation. It cannot tell you whether the affected pathway is conducting normally. Evoked potentials directly measure the functional conduction of the pathway - confirming that the structural lesion is actually impairing signal transmission, which is the clinically relevant question.
Localises the Lesion Within the Pathway
By recording the evoked response at multiple points along the sensory pathway simultaneously - peripheral nerve, cervical spine, brainstem, and cortex - SSEP can identify exactly where along the pathway conduction is impaired. This localisation helps determine whether a problem is peripheral or central, and at what level of the spinal cord a lesion is located.
Completely Non-Invasive
Unlike EMG, which requires needle insertion into muscle, all three evoked potential tests use only surface electrodes applied with conductive paste to the scalp and skin. There are no needles, no electrical stimulation to the head, no pain, and no risk beyond minor scalp electrode preparation. The tests can be performed in patients who are asleep, sedated, or under general anaesthesia - making them available for patient populations where cooperation with other diagnostic tests is not possible.
Clinical Presentations That Indicate Evoked Potential Testing
Evoked potential testing is indicated when clinical symptoms or the clinical question involves the integrity of the central sensory pathways - or when peripheral nerve testing has not provided a complete explanation of the patient's symptoms.

Neurological & Musculoskeletal Conditions Assessed with Evoked Potentials
Multiple Sclerosis (MS)
Cervical Myelopathy
Optic Neuritis
Acoustic Neuroma
Spinal Cord Injury
Peripheral Neuropathy (Large Fibre)
MVA CNS Pathway Documentation
Dizziness & Balance Disorders
Thoracic Outlet Syndrome
Brachial & Lumbosacral Plexopathy
Demyelinating Disease
Syringomyelia
What to Expect During Evoked Potential Testing at Dynamic PT
Preparation - Hair and Skin
Wash your hair thoroughly on the morning of the test and do not apply any hair products, gels, or sprays afterward. Wash your skin thoroughly and do not apply lotion, cream, or moisturiser. Clean, product-free scalp and skin are essential for electrode conductivity and accurate waveform recording. Wear comfortable, loose-fitting clothing. No fasting required - eat normally and take all medications as usual.
Electrode Placement
Your technician will gently clean small areas of your scalp with a mild abrasive gel to improve conductivity, then apply surface electrodes using a conductive paste that washes out easily with water. For SSEP, additional electrodes are placed at the wrist, ankle, or knee. For VEP and BAER, scalp electrodes only are required. The paste may feel slightly sticky but causes no discomfort, and all electrodes are removed at the end of the session.
The Stimulus Phase - Relaxed and Passive
For SSEP: a mild electrical tingling at the stimulation sites on your wrist or ankle is delivered repeatedly - hundreds of times - while you remain still and relaxed. For VEP: you watch a flickering checkerboard pattern on a monitor, one eye at a time, while remaining still. For BAER: you listen to clicking sounds through headphones while resting - you may even fall asleep during this component, which does not affect the results.
Signal Averaging and Waveform Generation
The evoked potential technique uses signal averaging - the brain's response to each stimulus is small and would be lost in background electrical noise. By repeating the stimulus hundreds of times and averaging the responses, the consistent evoked response is amplified while random noise cancels out. This is why each test requires several hundred stimulus repetitions and takes 30 - 60 minutes to complete.
Results, Interpretation & Integration
Your results are reviewed and discussed with you following the testing session. A written report documenting latencies and amplitudes of each measured waveform, comparisons to normative values, and clinical interpretation is generated for your physician and your legal team if applicable. The findings are integrated into your overall diagnostic picture and rehabilitation plan at Dynamic PT.
What Evoked Potential Testing Adds to Your Diagnostic Evaluation
Completely Non-Invasive
All three evoked potential tests use only surface scalp and skin electrodes. No needles, no injections, no electrical stimulation to the head. Safe for all patient populations including children, elderly, pregnant patients, and those with bleeding disorders or on blood thinners.
Detects Silent CNS Lesions
Evoked potentials can identify demyelinating lesions in the spinal cord and optic nerve before they produce clinical symptoms - a critical capability in MS diagnosis where demonstrating dissemination in space requires objective evidence from multiple CNS locations.
Objective Medico-Legal Documentation
For motor vehicle accident patients, evoked potential studies provide objective, reproducible, machine-generated documentation of central nervous system pathway disruption - the standard electrodiagnostic evidence required for personal injury claims involving neurological injury.
In-Clinic, Same-Day Integration
Testing is performed in our clinic and results are reviewed immediately - no separate neurology lab appointment, no waiting weeks for results. Findings are integrated directly into your PT diagnosis and treatment plan, or expedited to your referring physician and legal team.
Evoked Potential Testing FAQs
Are evoked potential tests painful?
The VEP and BAER tests involve no physical stimulus to the body whatsoever - you simply watch a screen or listen through headphones. These tests are completely painless. The SSEP test involves mild electrical stimulation to the wrists and/or ankles - similar to the sensation of a static electricity discharge or a brief tingle. The stimulus is well below the threshold for pain; it produces a mild, momentary tingling that most patients find only mildly uncomfortable at most. The scalp electrode application involves gentle skin preparation with a mildly abrasive gel - not painful, though slightly unusual in sensation. Overall, evoked potential testing is consistently rated as much more comfortable than needle EMG testing.
How is an evoked potential test different from an EEG?
Both tests use scalp electrodes to measure the brain's electrical activity - but they measure different things. An EEG (electroencephalogram) records the brain's spontaneous, continuous electrical activity, looking for abnormal patterns such as seizure activity. Evoked potential tests record the brain's specific, time-locked response to a defined sensory stimulus - the response to a specific sound, visual pattern, or electrical stimulus delivered in a controlled way. The evoked response is extracted from the background EEG noise by signal averaging. EEG answers "what is the brain doing spontaneously?" - evoked potentials answer "how quickly and how strongly does the brain respond to this specific sensory input?"
Why do I need an evoked potential test if I've already had an MRI?
MRI reveals anatomy - structural lesions, disc herniations, demyelinating plaques, tumours. What MRI cannot show is whether those structural findings are actually impairing the functional conduction of the nerve pathway. A patient may have a plaque on MRI that looks significant but is functionally silent - the pathway is conducting normally. Conversely, a patient may have a functionally significant conduction delay in their optic nerve with a completely normal MRI. Evoked potentials measure function, not structure. In MS particularly, combining MRI and evoked potentials is essential - each modality captures a different dimension of the disease, and together they provide a far more complete diagnostic picture than either test alone.
I was in a car accident and my attorney requested an evoked potential study. What does that mean?
In motor vehicle accident personal injury cases, evoked potential studies (particularly SSEP and BAER) provide objective, machine-generated documentation of nervous system pathway injury that cannot be faked, coached, or subjectively influenced by the patient. Unlike subjective pain reports or even clinical examination findings, evoked potential waveforms are purely physiological measurements - either the nerve pathway conducts normally in the expected time, or it doesn't. This objectivity makes evoked potential studies powerful evidence in personal injury litigation. If your attorney or treating neurologist has requested this testing, it is to document the extent and nature of neurological injury sustained in the accident with reproducible, objective data. Dynamic PT provides written reports suitable for submission to legal proceedings and insurance carriers.
Is evoked potential testing covered by insurance?
SSEP, VEP, and BAER testing is covered by Medicare, Medicaid, Workers' Compensation, and most commercial insurance plans when medically indicated - billed under evoked potential procedure codes as diagnostic studies. No-Fault coverage (motor vehicle accidents) frequently covers all three evoked potential tests as part of the neurological diagnostic work-up for MVA-related injury claims. Coverage is typically strong because these are established, recognised diagnostic procedures with clear clinical indications. At Dynamic Physical Therapy, we verify your specific diagnostic testing benefits before your appointment. Call (718) 826-3200 and our team will confirm your coverage.
